When melanoma is caught early, the chance of surviving five years or more is over 99%. But if it spreads to other organs, that number drops to just 32%. This isn’t just a statistic-it’s the difference between living a full life and facing a life-threatening illness. Melanoma doesn’t always look like a dark, uneven mole. Sometimes it’s a tiny spot that doesn’t heal. Other times, it’s a streak under a fingernail or a new bump that grows slowly. The problem? Most people don’t know what to look for. And even doctors can miss it without the right tools.
How Melanoma Is Detected Today
The old way of checking for melanoma? A visual exam. A doctor looks at your skin, maybe uses a magnifying tool called a dermoscope. But studies show this method catches only 60-70% of melanomas. That means nearly 1 in 3 cases are missed. It’s not because doctors aren’t careful-it’s because melanoma can hide in strange places and look like harmless moles.
Now, new technologies are stepping in. One of the most promising is a handheld device called DermaSensor. Approved by the FDA in early 2024, it uses near-infrared light to scan skin lesions. It doesn’t need a specialist. A family doctor can use it after just 2-3 hours of training. In trials, 87% of primary care providers said it gave them more confidence in their diagnosis. But here’s the catch: its specificity is only 26-40%. That means it flags a lot of harmless spots as suspicious. More biopsies. More anxiety. More cost.
Then there’s AI. Not the kind you see in movies-this is real, trained on hundreds of thousands of real skin images. Systems like SegFusion from Northeastern University combine two AI models: one that outlines the exact shape of a mole, and another that decides if it’s cancerous. It hits 99% accuracy. On the ISIC 2020 dataset-where melanoma made up only 1.8% of images-it still performed flawlessly. Why? Because it didn’t just learn from what melanoma looks like. It learned how to isolate it from everything else.
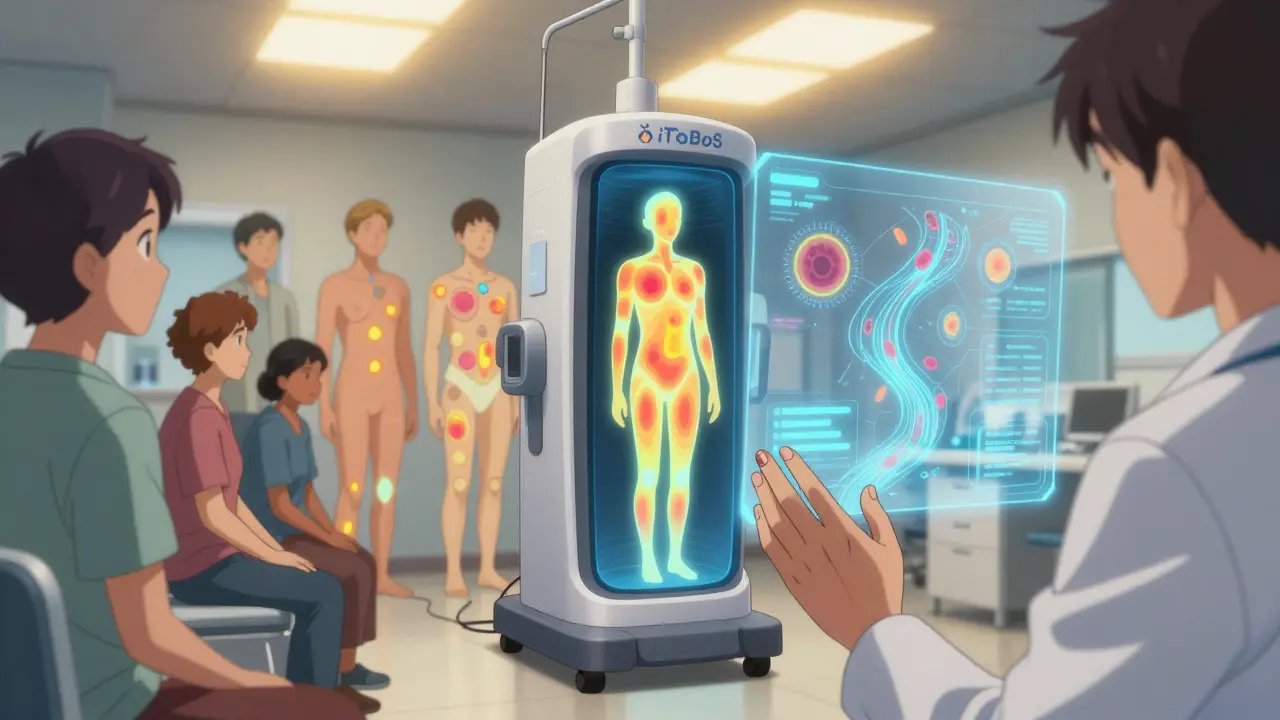
Full-body scanners are another breakthrough. The iToBoS project, backed by 20 European research teams, can scan a person’s entire skin in six minutes. It maps every spot, tracks changes over time, and flags risks with explainable AI. That means the system doesn’t just say “cancer”-it shows the doctor exactly why it thinks so. This is huge. Doctors don’t trust black boxes. They need to understand the logic.
The Hidden Problem: Bias in AI
Here’s something no one talks about enough: most AI systems for skin cancer were trained mostly on light skin. A 2025 JAMA Dermatology study found these tools are 12-15% less accurate on darker skin tones. That’s not a small gap. It’s life or death. A dark spot on a Black patient might be melanoma. But if the AI doesn’t recognize it because it was never trained on that skin type, the patient gets sent home with a “probably harmless” label. And that’s deadly.
Some companies are fixing this. SegFusion and iToBoS now include diverse datasets. But many commercial tools still don’t. If you’re using an AI tool, ask: Was it tested on people with different skin tones? If the answer is no, it’s not reliable for everyone.
What’s Coming Next
Wearable patches are on the horizon. Researchers at Wake Forest built a battery-free, wireless patch that sticks to the skin. It measures electrical differences between healthy tissue and cancerous cells. In a small trial with 10 volunteers, it found clear differences. The next version will use conductive hydrogel to stick better. Imagine checking your skin at home every week-no clinic visit needed.
And it’s not just about images. The future is multimodal. Combining AI scans with bioimpedance, genetic markers, even blood tests. One study is already testing whether adding oxygen levels and blood pressure data improves AI predictions. If it works, a simple skin scan could be paired with a quick health profile to give a much clearer picture.
Immunotherapy: Turning the Body Against Cancer
If melanoma spreads, surgery isn’t enough. That’s where immunotherapy comes in. Before 2011, metastatic melanoma was almost always fatal. Now, it’s treatable. And in many cases, curable.
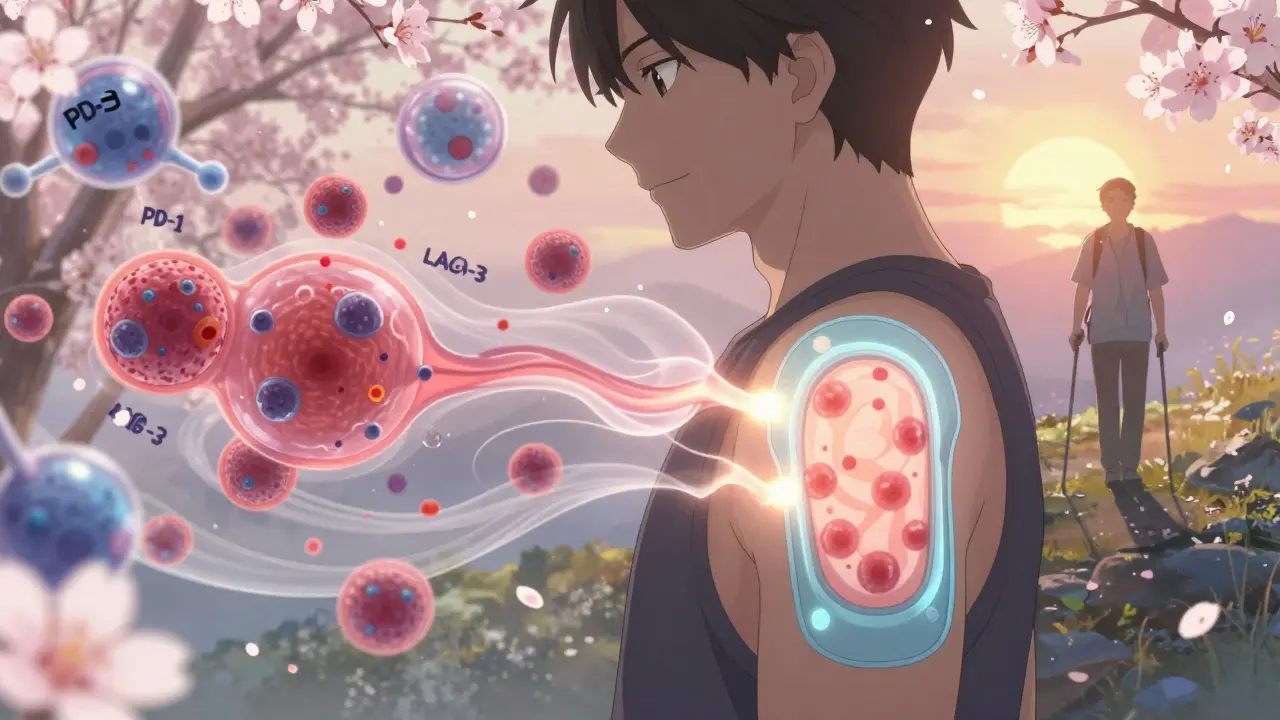
The first big breakthrough was ipilimumab, a drug that blocks a protein called CTLA-4. It woke up the immune system to attack cancer. Then came pembrolizumab and nivolumab-drugs that block PD-1. These were game-changers. Today, the standard is combination therapy: a PD-1 blocker plus a CTLA-4 blocker. This combo works better than either drug alone. In clinical trials, over half of patients with advanced melanoma saw their tumors shrink. Some disappeared completely.
Now, the next wave is here. Regeneron is testing a new combo: a PD-1 blocker with fianlimab, which targets LAG-3, another immune checkpoint. Early results show even deeper responses. And then there’s IMA203 PRAME cell therapy-a personalized treatment that trains a patient’s own immune cells to hunt melanoma. In Phase 1b, 56% of patients had no detectable cancer after treatment. It’s not approved yet, but the data is strong.
Immunotherapy isn’t perfect. Side effects can be serious: fatigue, rashes, even inflammation of the lungs or liver. But compared to chemotherapy? It’s a win. And for many, it means living years longer than anyone expected.
Real-World Challenges
These tools sound amazing. But getting them into clinics? That’s the hard part.
Integration takes time. Dermatology offices report needing 15-20 hours of training just to use one AI system. DermaSensor? Only 2-3 hours. But if the system doesn’t plug into your electronic health records, doctors won’t use it. And right now, 76% of providers say integration is a nightmare.
Then there’s cost. The FDA approves AI tools, but insurance doesn’t always cover them. Google Health pulled its AI tool from the market in late 2024 because reimbursement was too low. If doctors can’t get paid for using it, they won’t use it.
And there’s overdiagnosis. A 2025 study warned that screening too aggressively might catch tiny melanomas that would never harm anyone. More biopsies. More scars. More stress. The goal isn’t to find every single mole. It’s to find the dangerous ones-and leave the rest alone.
What You Can Do
You don’t need a high-tech scanner to save your life. Here’s what works right now:
- Check your skin monthly. Use the ABCDE rule: Asymmetry, Border irregularity, Color variation, Diameter over 6mm, Evolving size or shape.
- Don’t ignore spots that bleed, itch, or don’t heal.
- If you have a family history of melanoma or many moles, see a dermatologist yearly.
- Ask your doctor: Do you use any AI tools for skin checks? Are they tested on diverse skin tones?
- Protect your skin daily. UV exposure is the #1 cause. Wear sunscreen, hats, and avoid tanning beds.
Early detection saves lives. But detection alone isn’t enough. We need better tools, fairer AI, and access for everyone-not just those who can afford it.
The Future Is Here
By 2030, AI-assisted melanoma detection will likely be standard. Immunotherapy will keep improving. Survival rates will rise. But progress won’t be automatic. It needs investment. It needs diversity in data. It needs policy changes. And it needs patients to speak up.
This isn’t science fiction. It’s happening now. In Sydney, in Berlin, in Cleveland. In clinics using AI to spot cancer before it spreads. In labs designing patches that could one day be sold at pharmacies. In trials where patients are beating odds no one thought possible.
The message is simple: If you see something strange on your skin, don’t wait. And if you’re a doctor-ask: Is your tool helping everyone, or just some?
Can melanoma be detected before it becomes dangerous?
Yes. When caught at the earliest stage-before it spreads beyond the skin-the five-year survival rate is over 99%. Tools like dermoscopy, AI image analysis, and wearable sensors can identify suspicious lesions before they turn into advanced cancer. Regular self-checks and annual skin exams with a dermatologist are the most effective ways to catch melanoma early.
Is immunotherapy better than chemotherapy for melanoma?
For most advanced melanoma patients, yes. Immunotherapy works by helping the body’s own immune system attack cancer cells, while chemotherapy poisons fast-growing cells-including healthy ones. Immunotherapy has fewer side effects and longer-lasting results. In fact, some patients remain cancer-free for over a decade after treatment. Chemotherapy is now mostly used when immunotherapy doesn’t work.
Do AI skin scanners work for all skin tones?
Not all of them. Many AI systems were trained mostly on light skin, so they’re less accurate on darker skin tones-up to 15% less accurate, according to a 2025 study. Always ask if the tool you’re using was tested on diverse populations. Systems like SegFusion and iToBoS include diverse data and perform better across skin types.
Can wearable patches replace doctor visits?
Not yet. Wearable patches, like the one from Wake Forest, show promise for at-home monitoring, but they’re still in early testing. They can flag changes, but they can’t replace a biopsy or clinical diagnosis. Think of them as early warning systems-not final answers.
What’s the biggest risk with new melanoma detection tech?
Overdiagnosis. Some tools, especially those with low specificity, flag too many harmless spots as cancerous. This leads to unnecessary biopsies, anxiety, and costs. The goal isn’t to find every mole-it’s to find the ones that will become dangerous. That’s why combining tools with clinical judgment is critical.


14 Comments
Scott Easterling
10 March, 2026Let me guess-this is just Big Pharma and Silicon Valley’s latest money grab. 🤡 They want you scared so you’ll pay $500 for a ‘smart’ dermoscope that’s 40% accurate. Meanwhile, real doctors who’ve been doing this for decades are being sidelined by algorithms trained on white people’s skin. And don’t even get me started on how they’re pushing these patches… next thing you know, the government’s scanning your backyard for ‘suspicious moles.’
Remember when they said vaccines were safe? Now we know better. Same playbook. Fear. Tech. Profit. You’re being played.
Mantooth Lehto
10 March, 2026I just cried reading this. 😭 My sister died of melanoma because her doctor said ‘it’s probably just a mole.’ I’ve been checking my skin every day since. I even took pics of every spot. I’m not taking chances anymore. If you have a mole that won’t go away… GO. TO. A. DOCTOR. No excuses. I lost my sister. Don’t lose yours.
Melba Miller
11 March, 2026AI? In America? Please. We can’t even get decent healthcare for veterans, and now you want us to trust a machine built in a lab that’s never seen a Black person’s skin? This isn’t innovation-it’s colonialism with a USB port.
And don’t tell me ‘SegFusion is inclusive.’ I’ve seen the data. The ‘diverse dataset’ they brag about? 3% of their training images were from people of color. That’s not inclusion. That’s tokenism. And it kills.
Meanwhile, in the U.S., insurance won’t cover a $200 scan but will pay $12,000 for chemo. We’re not fixing the system. We’re just slapping on a shiny new bandage.
Neeti Rustagi
12 March, 2026While the technological advancements in melanoma detection are indeed commendable, one must also consider the ethical implications of algorithmic bias in medical AI systems. The lack of representation in training datasets is not merely a technical oversight-it is a systemic failure that disproportionately endangers marginalized populations.
Furthermore, the integration of AI tools into primary care settings must be accompanied by robust regulatory frameworks and equitable reimbursement policies. Without these, innovation risks exacerbating existing disparities rather than alleviating them.
It is imperative that stakeholders prioritize inclusivity, transparency, and accessibility in the deployment of these tools.
Dan Mayer
14 March, 2026wait so ai is 99% accurate?? lol no way. they just trained it on like 500 pics and called it a day. also who even has time to get a full body scan? i work 2 jobs. and why are they using ‘explainable ai’ like that’s some miracle? it’s still a black box. also i think they just made up the 87% stat. i’ve seen docs use these things and they’re always like ‘uhhh idk’
Janelle Pearl
15 March, 2026Thank you for writing this. I’ve been terrified of skin checks since my mom passed. But reading this? It made me feel less alone.
I do monthly checks. I’ve started taking selfies of my back and legs. I don’t wait for ‘something to change.’ I go in if something feels off-even if it looks fine.
And yes, I asked my derm if their AI tool was tested on darker skin. She said no. So I switched providers. It’s not easy. But I owe it to myself.
Robert Bliss
16 March, 2026Just want to say I’m glad we’re talking about this. I’ve had 3 biopsies in 5 years. All benign. But I’d rather be safe than sorry. I don’t trust AI 100%, but I do trust the combo of a good doc + a good tool. And yes-sunscreen. Every. Single. Day. Even in winter. 💪
Peter Kovac
16 March, 2026The data presented is statistically incoherent. The claim of 99% accuracy on the ISIC 2020 dataset is misleading without context of class imbalance. With melanoma representing only 1.8% of samples, high accuracy is trivial. Sensitivity and specificity must be reported together. Furthermore, the 26-40% specificity of DermaSensor renders it clinically unusable without confirmatory biopsy. This article is a disservice to evidence-based medicine.
Erica Santos
17 March, 2026Oh wow. So we’re just gonna let a bunch of nerds in Silicon Valley decide who lives and who dies based on how their skin reflects infrared light? Classic. Next up: AI that tells you if your child is ‘emotional enough’ to deserve therapy. 😏
Meanwhile, in 2025, the CDC still can’t get sunscreen on the医保 list. But sure-let’s fund a $10,000 scanner for the 1%.
George Vou
18 March, 2026they say immunotherapy works but i read somewhere the side effects are worse than the cancer. like your body starts eating itself. and what about the people who can’t afford it? i mean if you’re poor and get melanoma… you’re basically dead. also why is everyone so into ai? i just want a good doc who knows what they’re doing. not a robot.
Katy Shamitz
20 March, 2026My cousin got diagnosed because she noticed a tiny spot under her toenail. No one believed her. She had to beg for a biopsy. It was melanoma. Stage 1. She’s fine now. But if she’d waited? Gone.
Stop ignoring weird spots. Even if they’re ‘small.’ Even if they’re ‘not black.’ Even if your doctor says ‘it’s nothing.’ Trust your gut. I’m telling you-this isn’t drama. It’s survival.
Nicholas Gama
22 March, 2026Wearable patches? Cute. But let’s be real: if you can’t afford a dermatologist, you can’t afford a patch. This isn’t innovation. It’s luxury healthcare repackaged as ‘democratized tech.’ The real solution? Universal access. Not gadgets.
Mary Beth Brook
23 March, 2026Overdiagnosis is a myth perpetuated by anti-screening lobbies. The data shows early detection reduces mortality by 63%. The real issue is underdiagnosis in underserved populations. Stop using ‘overdiagnosis’ as a shield to avoid equity reform. If the tool flags a lesion, it’s not the tool’s fault-it’s the system’s.
Scott Easterling
23 March, 2026Wow. Someone actually replied to my comment. That’s a first. Anyway-your sister? She was a victim of the system. But so are you. You’re checking your skin daily? That’s not vigilance. That’s trauma. And they’re selling you more scans to keep you scared. You don’t need a scanner. You need justice.